Evidence suggests that neuroactive steroids may be candidate modulators of schizophrenia pathophysiology and therapeutics.
We therefore investigated neuroactive steroid levels in post-mortem brain tissue from subjects with schizophrenia, bipolar disorder, nonpsychotic depression, and control subjects to determine if neuroactive steroids are altered in these disorders.
Posterior cingulate and parietal cortex tissue from the Stanley Foundation Neuropathology Consortium collection was analyzed for neuroactive steroids by negative ion chemical ionization gas chromatography/mass spectrometry preceded by high-performance liquid chromatography.
Subjects with schizophrenia, bipolar disorder, nonpsychotic depression, and control subjects were group matched for age, sex, ethnicity, brain pH, and post-mortem interval (n = 14-15 per group, 59-60 subjects total). Statistical analyses were performed by ANOVA with post-hoc Dunnett tests on log transformed neuroactive steroid levels.
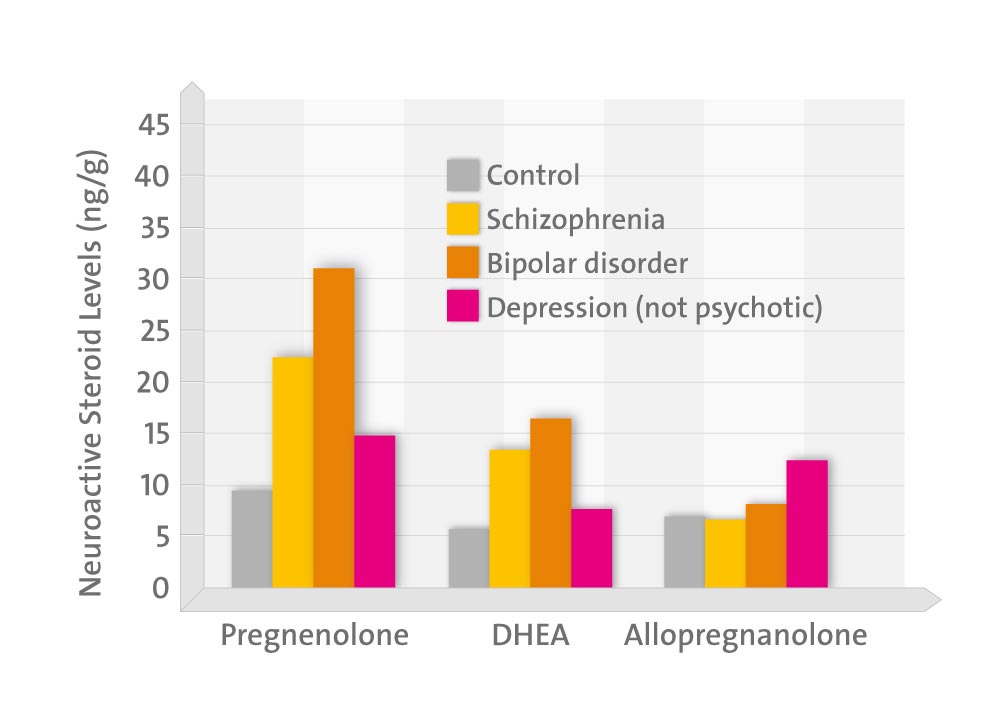
Pregnenolone and allopregnanolone were present in human post-mortem brain tissue at considerably higher concentrations than typically observed in serum or plasma. Pregnenolone and dehydroepiandrosterone levels were higher in subjects with schizophrenia and bipolar disorder compared to control subjects in both posterior cingulate and parietal cortex. Allopregnanolone levels tended to be decreased in parietal cortex in subjects with schizophrenia compared to control subjects.
Neuroactive steroids are present in human post-mortem brain tissue at physiologically relevant concentrations and altered in subjects with schizophrenia and bipolar disorder. A number of neuroactive steroids act at inhibitory GABA(A) and excitatory NMDA receptors and demonstrate neuroprotective and neurotrophic effects. Neuroactive steroids may therefore be candidate modulators of the pathophysiology of schizophrenia and bipolar disorder, and relevant to the treatment of these disorders.